Patient Ombudsman Years 4 & 5
Courage
Compassion
Clarity
Informing change in a time of crisis


Remembering Cathy Fooks
A legacy of unparalleled dedication to excellence in health care and patient experience.
A tribute to Cathy

Remembering Cathy Fooks
Cathy Fooks was appointed as Ontario’s second Patient Ombudsman on July 13, 2020 and led the office until her passing on December 30, 2020. Her integrity, kindness, humour and unparalleled dedication to excellence in health care and patient experience left a lasting legacy. She continues to inspire the office’s work and commitment to ensure that every experience counts.
Donate to the Cathy Fooks Award for Research and Leadership Excellence in Patient and Caregiver Engagement
This award supports DLSPH and IHPME non-professional Master or doctoral students, who contribute to the evidence-base for patient and caregiver engagement in the health system, including evaluation and measurement strategies.
Make a giftPatient Ombudsman’s message
Meeting an ever-growing demand for help navigating a health care system that is increasingly complex and continuously evolving.
Craig Thompson’s message

Patient Ombudsman’s message
As Ontario’s Patient Ombudsman, it is my privilege to share this annual report with our stakeholders. It would be an understatement to say that the last two years have been challenging. The impact of the COVID-19 pandemic can be seen throughout this report, both in the information presented and the stories shared. But even with the pandemic and other challenges we faced, this nascent office remained focused on meeting an ever-growing demand for help navigating a health care system that is increasingly complex and continuously evolving.
Committed to Listening, Learning and Leading
The vision for Ontario’s first health ombuds office was to be a trusted champion for fairness and to influence positive change in the health care system. Bringing that vision to life requires listening to the stories of patients and caregivers who rely on our system for their care and listening to the health care organizations and the dedicated professionals who work to provide the care. Only then can we fully understand the issues and arrive at recommendations that serve to bring about change so that others have more positive health care experiences.
To do this, our office is guided by a set of values that inform how we work. We respect the dignity, privacy and diversity of every person who comes to us and take the time to listen closely and carefully, acknowledging all experiences and perspectives. We communicate clearly in a professional, courteous way that respects all people, languages and abilities. We treat people fairly and look at every issue impartially, listening to all sides. We are empathetic and acknowledge that every experience is unique, while responding with openness and compassion. We strive to be trustworthy and accountable to the people we serve and to provide high-quality service that adapts and improves as we learn.
At its most fundamental, the work of an ombuds involves looking at what was decided, how it was decided and how people were treated before deciding if an organization acted fairly. Over the last five years, the Patient Ombudsman team has developed considerable expertise in assessing fairness, resulting in resolutions that are trusted and respected by all parties. Ideally fairness in decision-making and service delivery would be considered at the outset – when health sector organizations are designing policies and programs – so that the issues that typically give rise to complaints to our office don’t occur. The ‘fairness by design’ concept is championed by many in Canada’s ombuds community, and I wholeheartedly support this proactive approach to achieving fairness.
Hardship and Heartbreak
The COVID-19 pandemic has created no end of hardship – from the loss of loved ones and time with friends and family, to the loss of freedoms we took for granted. In our first of three special reports that look at the impact COVID-19 had on resident, patient and caregiver experiences, we aimed to quickly distill the insights from the complaints we received and reflect them back to the health care system to inform pandemic planning and decision-making. The office’s ability to pivot and adjust to the challenges brought on by the pandemic is something the Patient Ombudsman team should be enormously proud of.
It was also during the pandemic that our office suffered the heartbreaking loss of our ombuds, Cathy Fooks, who passed away December 30, 2020. Cathy was a highly respected health care leader, mentor, and irrepressible champion of patients and caregivers who pushed for changes to improve the health care system for us all. We keep Cathy, her family, and her many friends and colleagues in our hearts and thoughts as we continue this important work.
Important Milestones
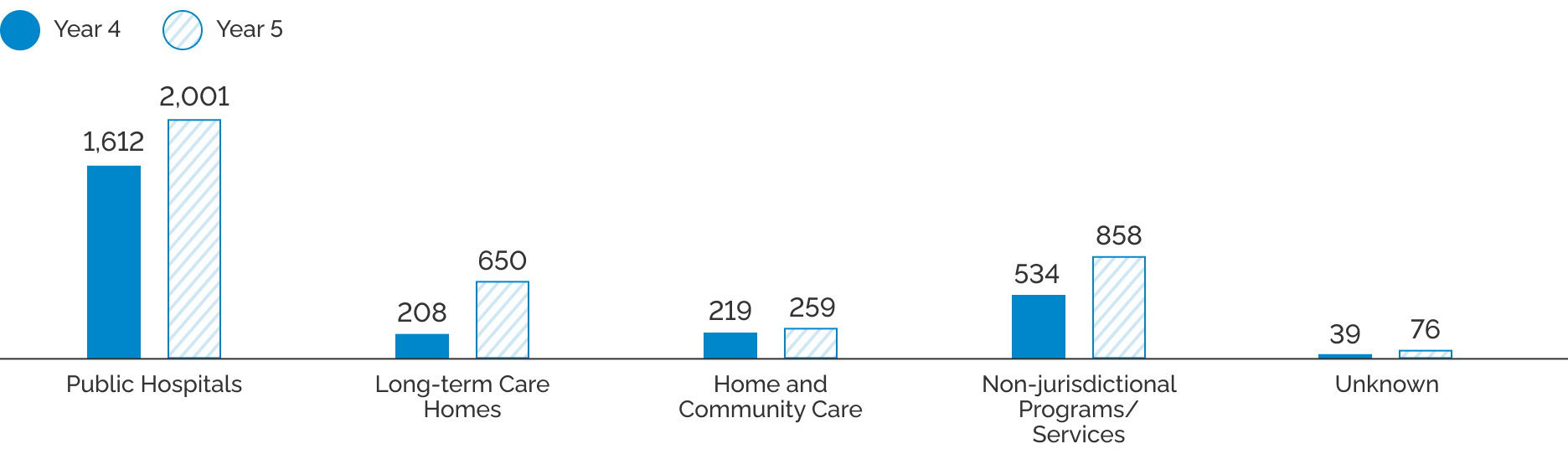
Overall, complaints to the office have been increasing since the office opened. As the largest health care sector, hospitals typically make up the bulk of complaints followed by long-term care and home and community care. By the end of April 2020, the office was receiving a disproportionate number of complaints about long-term care homes, pointing to the unfolding crisis in that sector. The office responded by issuing its first public call for complaints, initiating targeted outreach to key stakeholders as well as launching its first large-scale, system-level investigation of the impact of COVID-19 on the health care experience of long-term care home residents.
The initiation of a large-scale, system-level investigation was an important milestone for this office, and I look forward to sharing the results of that investigation in 2022. Through our broader investigative work and as you will see in the summary of our investigation on breakdowns in coordinated care, we have identified where gaps in oversight can make it challenging to comprehensively investigate a complainant’s entire health care experience and deliver recommendations that speak to the full continuum of care. It should be a priority for all of us who are committed to improving the health care system to find ways to close these gaps, so patients and their loved ones are not caught in the middle.
The ability to report on the nature of complaints and the insights they provide is key to having impact as an ombuds. While the pandemic dominated much of the Patient Ombudsman’s work during years 4 and 5, we continued to adjust our processes and invest in technology to increase our data collection and analysis capabilities so that we can report on the full breadth of health care experiences including the experiences of patients and caregivers who face challenges accessing health care due to racism, bigotry and intolerance.
Looking to the Future
When I took up my duties as Ontario’s third Patient Ombudsman on March 29, 2021, I did so with the support of an exceptional team of professionals who, like me, are drawn to helping people navigate a health care system that, at times, seems anything but fair. Their hard work and dedication over these two years has allowed our office to not just survive but to also thrive.
I want to recognize the courage of the residents, patients, and caregivers who brought their concerns to us while also seeking compassion, understanding and support. I also want to recognize the thousands of professionals who work in Ontario’s health care system; you have my gratitude and respect for the care you provide, sometimes under extremely challenging circumstances.
I welcome your thoughts, ideas, and insights from what you learn in this annual report.
Sincerely,
Craig Thompson
Patient Ombudsman
How we got here
5 years of impact
Patient Ombudsman opened its doors and phone lines on July 4, 2016 and began receiving complaints from patients (including long-term care home residents) and caregivers about their health care experiences. Over the last five years, we have worked hard to champion fairness in health care and listen to patients, caregivers and health sector organizations (HSOs).
“I am very pleased with the resolution. And I thank you for being a part of this process. I have not wanted to cause any trouble or grief, I just want to be cared for medically, the same as everyone else is…This resolution is exactly what I was hoping and looking for…I always felt that you truly cared about me and what I was going through.”
The Patient Ombudsman’s authority is set out in the Excellent Care for All Act, 2010. Our role is to receive, respond to and help resolve complaints from current or former patients or their caregivers about their care or experiences with HSOs. The HSOs within our jurisdiction currently include public hospitals, long-term care homes and home and community care support services organizations.
Over our first five years, Patient Ombudsman has evolved and developed our response to complaints to better meet the needs of Ontario patients and their caregivers. The foundation for our ongoing development was laid in our first three years with three significant accomplishments: the development of our first set of strategic aims and objectives; the development of the Fairness Triangle; and our Service Charter.
Complaint overview
Record numbers, unique challenges
At the end of March 2020, Patient Ombudsman began tracking a significant increase in complaints about the impact of COVID-19 on Ontario’s long-term care homes. We reported weekly on complaints related to COVID-19 and shared our reports with health system leaders. The complaints highlighted serious concerns in long-term care homes, including inadequate infection prevention and control practices, lack of access to appropriate personal protective equipment, communication gaps and significant staff shortages that were affecting resident care.
Complaints
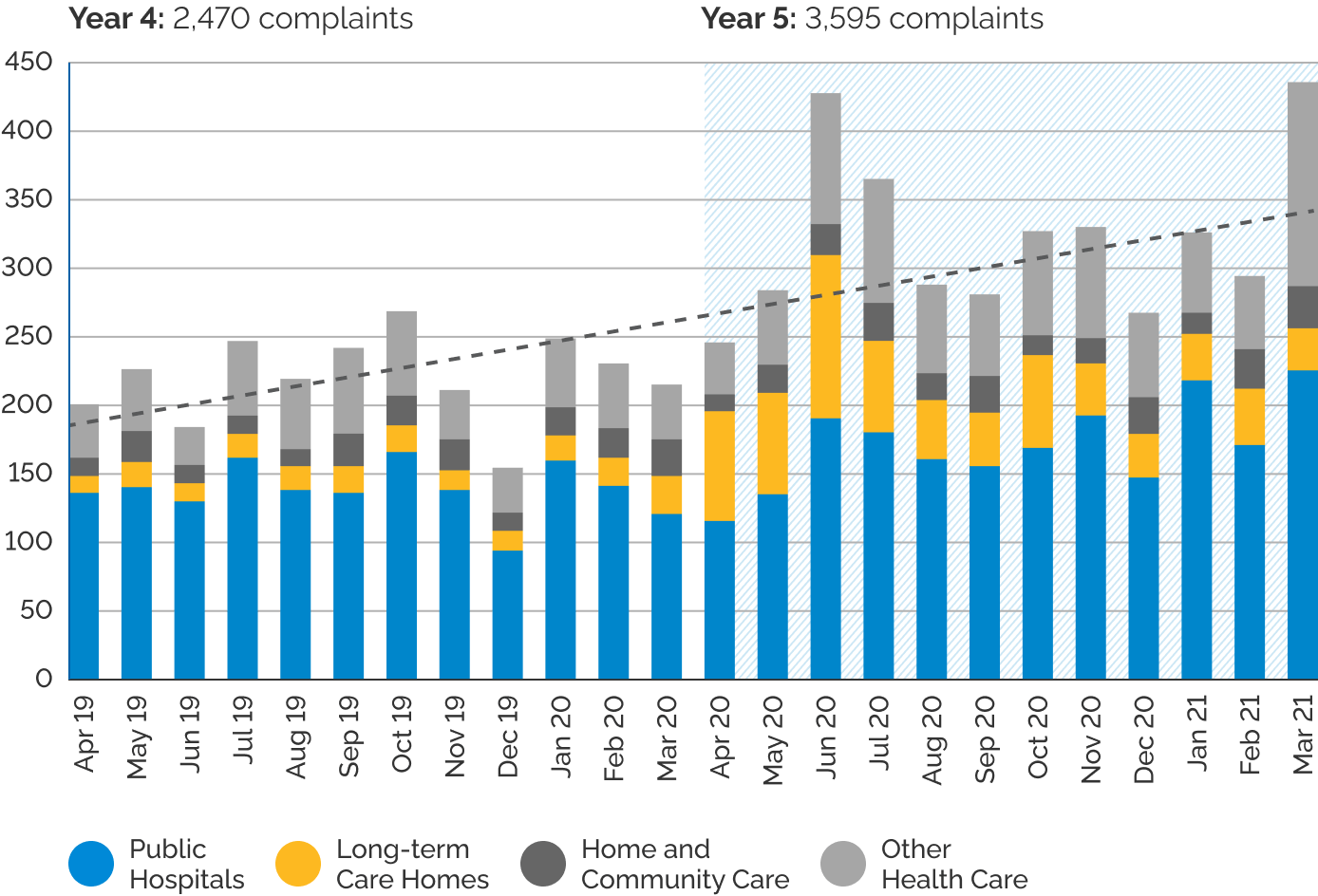
Complaints about long-term care homes typically make up less than 10% of the complaints received by Patient Ombudsman. By the end of April 2020, 33% of complaints were about long-term care homes. To gain a better understanding of the complexity of these concerns, Patent Ombudsman issued its first public call for complaints on April 27, 2020.
Impact of COVID-19 on the care and health care experience of long-term care home residents
Patient Ombudsman also launched its first large-scale, system-level investigation of the impact of COVID-19 on the care and health care experience of long-term care home residents in June 2020. The results will be released in 2022. In October 2020, Patient Ombudsman released the first of three special reports on the impact of COVID-19 on the experiences of patients and caregivers.
Read the first special reportSpotlight issues
Opportunities for improvement
Patient Ombudsman monitors the complaints we receive to identify emerging issues. Our “Spotlight” stories shine a light on the kinds of cases we receive, how we achieve resolutions, and where HSOs can look for opportunities to improve patient and caregiver experiences.