Patient Ombudsman is a champion for fairness in Ontario’s healthcare system.
In our third year, we continued to receive more complaints and achieved more resolutions to improve healthcare experiences for all Ontarians. We believe that all experiences matter and that complaints about healthcare provide important information that can drive positive change.
How we work
Patient Ombudsman is a young organization, and we often hear that people are not aware of the help we can offer when they have problems with their healthcare.
As we look forward to the appointment of a new Patient Ombudsman in 2020, we continue to reach out to patient and caregiver groups and health providers to raise awareness of our services.
In our third year Patient Ombudsman staff visited 7 communities across the province and met with 26 stakeholder groups. We are also committed to ongoing learning and skills development. We welcomed subject matter experts to enhance our internal expertise on just some of the following:
- Supporting Indigenous identified complainants as they navigate our complaints resolution service in a culturally competent manner
- Supporting our own staff to build their internal resilience as they work with complainants in distress and living with a mental illness
- Palliative care and advanced care planning initiatives in hospitals
- The structure of pain specialist clinics and referral processes coordinated by public hospitals, and
- Gleaning insight into the work and unique processes of other ombuds offices, regulatory colleges and oversight agencies.
As we work with patients, caregivers and health sector organizations to resolve their concerns and improve healthcare, we are also focused on improving the services we offer and are listening to the feedback we receive. In our first two years, we heard from some that our resolution process took too long.
This year, we undertook a comprehensive review of our internal processes to respond to what we heard and learned from the experience of our front-line team. We reviewed how complaints are received and managed by our office with a view to increasing efficiency and eliminating unnecessary steps. Based on what we learned, we completed a re-design of our complaint management information system and introduced the changes in June 2019. To ensure that we can continue to produce high quality data, we developed a data dictionary, introduced data quality audits and provided training for the Patient Ombudsman team.
Service Charter
We also heard that patients, caregivers and health sector organizations wanted to better understand how we work.
They wanted to know what they can expect from us, what we expect from them and how they can most effectively engage with us. We consulted with patient and caregiver advisory groups and patient relations representatives of health sector organizations to develop and implement a service charter that describes how we work with patients, caregivers and health sector organizations to find fair resolutions to complaints. The Patient Ombudsman Service Charter was introduced in the winter of 2019 and we have shared it widely with patients, caregivers and health providers.
Patients and caregivers


We will:
- Make sure that our service is easy to access
- Respect your experience
- Listen to your complaint and concerns
- Explain what we can do to help
- Direct you to the right place if we can’t help
- Seek a fair resolution to your complaint
- Keep you informed and communicate our decisions clearly
- Welcome your feedback so we can improve
You will:
- First try to formally resolve your complaint with the hospital, long-term care home, or Local Health Integration Network (LHIN) that you’re complaining about
- Share all important facts and information about your complaint
- Recognize we are impartial and are looking for fairness from all sides
- Contact us with questions about your complaint
- Treat us with respect
- Let us know how we could improve your experience with us
Health sector organizations
(Public hospitals, long-term care homes, and home care)


We will:
- Clearly explain our role, process and expectations
- Ensure you have a meaningful opportunity to resolve the complaint
- Work with you to set reasonable timelines
- Be thorough and fair in our review
- Ask for specific information (policies, evidence & documentation)
- Keep you informed and explain our decisions
- Be open to innovative and creative solutions
You will:
- Respect our staff, process and timelines
- Explain your process and decisions
- Provide the information we ask for
- Contact us with any questions or concerns
- Respond to our suggestions and recommendations
- Let us know how we can improve your experience with us
Results in our third year
Patient Ombudsman received a total of 2,419 complaints in our third year, a 5% increase over the previous year. This includes 1,766 complaint enquiries received by phone or in-person and 653 formal written complaints.
As in our first two years, the majority (62%) of complaints about health sector organizations within Patient Ombudsman’s mandate were about public hospitals. This was followed by home and community care coordinated by Local Health Integration Networks (LHINs) (9%) and long-term care homes (8%).
18% of complaints were about health care services and providers that are outside of Patient Ombudsman’s jurisdiction. Complaints are often complex and involve many issues, some of which are within the Patient Ombudsman mandate and others that fall under the mandate of other oversight bodies, such as health professional regulatory colleges, the Information and Privacy Commissioner or the Ontario Ombudsman. Patient Ombudsman carefully analyzes each complaint to ensure a comprehensive response. When appropriate, Patient Ombudsman helps patients and families to navigate to a body or organization that can address their concern or parts of it. Our advice is, if you’re not sure, call us. If we can’t help, we’ll try to find someone who can. In all, Patient Ombudsman made over 2,000 referrals to other organizations, professional colleges and other resources to help patients and caregivers fully resolve their complaints. However, for some complainants, there is no one that provides independent oversight over their concerns—a consideration for future planning.
In our third year, a significant proportion, 267 (11%) of complaints were from patients and caregivers who raised concerns about access to or experiences with mental health and addictions services. Many of these complaints were from patients and caregivers who experienced delays or a lack of specialized services in their communities. We also heard from people who had difficulty accessing other health services, such as primary care, as a result of their mental health conditions.
Patient Ombudsman will continue to monitor and report on our mental health and addictions related complaints.
All complaints



Total number of complaints per 100,000 residents for each of the 14 Local Health Integration Network regions
(based on 1,844 complaints with known locations)
This year we looked at the geographic distribution of complaints across health regions, and found that a number of complaints we received, adjusted by the size of the local population, varied widely across the province. We will continue to examine these results and use them to help plan our outreach to communities across the province over the coming year.
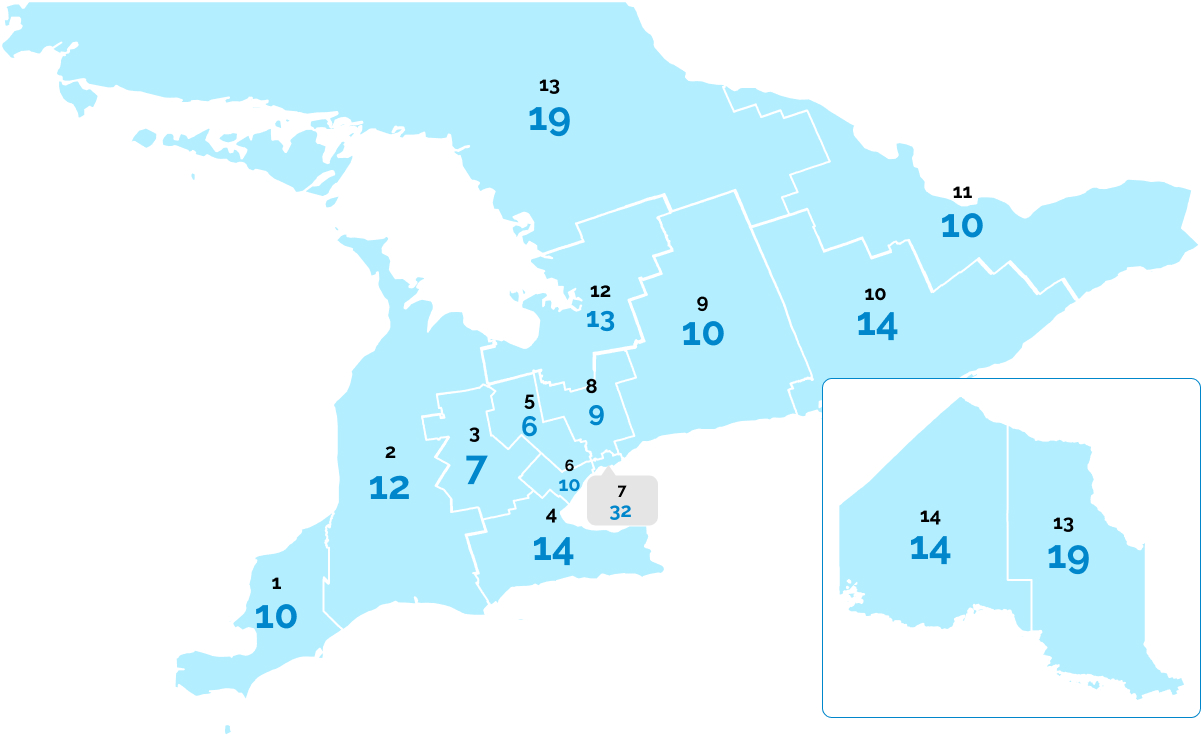
- Region 1 Erie St. Clair: 10
- Region 2 South West: 12
- Region 3 Waterloo Wellington: 7
- Region 5 Central West: 6
- Region 6 Mississauga Halton: 10
- Region 7 Toronto Central: 32
- Region 8 Central: 9
- Region 9 Central East: 10
- Region 10 South East: 14
- Region 11 Champlain: 10
- Region 12 North Simcoe Muskoka: 13
- Region 13 North East: 19
- Region 14 North West: 14
Complaint enquiries (phone or in-person)
Only 112 of the 1,766 patients and caregivers who initially made a complaint enquiry with Patient Ombudsman by phone went on to submit a formal written complaint, suggesting that the majority of complaints were resolved without the need for a formal complaint once contact with a member of our team was established.


Formal complaints (written)
The regulations guiding Patient Ombudsman require complaints to be submitted in writing. As noted above, Patient Ombudsman works to resolve all of the complaints we receive, but responding to formal written complaints makes up the majority of our efforts.
Looking more closely at the 653 formal written complaints Patient Ombudsman received, 11% involved health providers or services that are outside of our jurisdiction, and 22% concerned matters, such as the clinical decisions of health care professionals, that were more appropriately dealt by professional colleges or other bodies. In a further 28%, it was ultimately determined that the health sector body that was the subject of the complaint had not yet had a meaningful opportunity to address the complaint. In all of these cases, Patient Ombudsman counselled complainants, provided information and helped them to connect with someone who could help.





Patient Ombudsman also has the ability to undertake formal investigations of complaints that we are not able to resolve or other issues that have a public interest and fall within our mandate. In our third year, Patient Ombudsman undertook three investigations, each of which involved significant planning, review of hundreds of records and documents, and interviews with dozens of witnesses. Summaries of these investigations and the recommendations arising from our findings will be published in the coming months.
What did patients and caregivers complain about?
While the nature of complaints to Patient Ombudsman vary by sector, this year there were a number of common concerns about public hospitals, LHIN home and community care and long-term care homes. All three lists of the most frequent types of complaints include access or admission to services, concerns about communication and patient engagement, and complaints about health sector organizations internal complaint processes.
Complaints by Health Sector Organization
Top 10 types of complaints about public hospitals
Total number of complaints about public hospitals – 1,502
Legend
- 20%
- 14%
- 13%
- 12%
- 9%
- 9%
- 7%
- 5%
- 5%
- 5%
 See definition
See definition
 See definition
See definition
 See definition
See definition
 See definition
See definition
 See definition
See definition
 See definition
See definition
 See definition
See definition
 See definition
See definition
 See definition
See definition
 See definition
See definition
*Percentage of total complaints received about Public Hospitals.
Percentage of complaints by hospital group:
Top 10 types of complaints about home and community care
Total number of complaints about home and community care coordinated by LHINs - 226
Legend
- 23%
- 14%
- 13%
- 12%
- 11%
- 10%
- 6%
- 6%
- 4%
- 3%
 See definition
See definition
 See definition
See definition
 See definition
See definition
 See definition
See definition
 See definition
See definition
 See definition
See definition
 See definition
See definition
 See definition
See definition
 See definition
See definition
 See definition
See definition
**Percentage of total complaints received about LHIN home and community care.
Top 10 types of complaints about long-term care homes
Total number of complaints about long-term care homes – 194
Legend
- 19%
- 11%
- 10%
- 9%
- 8%
- 7%
- 6%
- 6%
- 5%
- 5%
- 5%
 See definition
See definition
 See definition
See definition
 See definition
See definition
 See definition
See definition
 See definition
See definition
 See definition
See definition
 See definition
See definition
 See definition
See definition
 See definition
See definition
 See definition
See definition
 See definition
See definition
***Percentage of total complaints received about LTC Homes.
How were complaints resolved?
In resolving complaints, Patient Ombudsman listens to all sides and works with complainants and health sector organizations to achieve a fair result.
In many cases, helping patients connect or re-connect with the patient relations representative at their health care organization is the best way to resolve their concern. Patient Ombudsman made almost 800 referrals and courtesy calls to patient relations representatives. In other cases, Patient Ombudsman determines that health sector organizations have already taken reasonable steps and no further action is required. In 128 cases, health sector organizations undertook improvements in response to a review that resulted in suggestions from Patient Ombudsman.
Patient Ombudsman received 120 complaints in year 3 from patients or caregivers who felt they had unfairly been charged co-payments or fees by hospitals or long-term care homes. Similar complaints were received in our first two years. To date, over $82,000 in fees have been voluntarily waived or reduced by health sector organizations following review by Patient Ombudsman.
Resolutions
128 cases
in which health sector organization made changes to address the concern brought forward by the patient or caregiver.
Over $82,000
in fees have been voluntarily waived or reduced by health sector organizations following review by Patient Ombudsman.
Over 2,000 referrals
made to other complaints bodies, provincial organizations or health services.
The Top 10 referrals:
Monitoring complaint trends and clusters
By monitoring and shining a light on trends and consistent clusters of complaints, Patient Ombudsman hopes to encourage health sector organizations to review their policies and practices and seek opportunities to improve the care experiences of patients and caregivers. This year Patient Ombudsman is highlighting four spotlight issues.